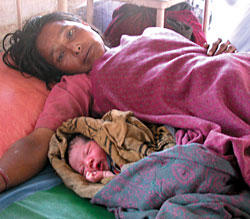
 Sanchita was too young for it all: married off in her teens, pregnancy, losing a child at birth and finally her own death before her 16th birthday.
Sanchita was too young for it all: married off in her teens, pregnancy, losing a child at birth and finally her own death before her 16th birthday.
When her labour pains came, Sanchita's in-laws refused to take her to the district hospital insisting on adhering to the family tradition of bearing children at home. She delivered her child without help from a trained birth attendant but the baby died soon after being born. Sanchita herself had lost a lot of blood and in the next few days, her condition deteriorated. The only medical aid she received were aspirins. After two weeks, the family finally decided to take her to a hospital. But it was too late.
That day earlier this year in mid-western Nepal, Sanchita became a statistic. She contributed to Nepal's shocking maternal mortality statistics which puts this country at the same level as sub-Saharan Africa.
Pregnancy related complications kill over 4,500 Nepali women every year, close to 12 deaths every day, one every two hours. The government's figures put Nepal's maternal mortality rate at 530 per 100,000 births but this is obviously a doctored figure. UNDP estimates it is closer to 740 and the Population Reference Bureau puts it even higher at 830 per 100,000 births. Compare this to Thailand with 44, Sri Lanka with 92 and Bangladesh with 380 mothers dying out of out of 100,000 births.
Whatever Nepal's figures for maternal mortality, it is clear that the situation for motherhood in Nepal is even bleaker because of the conflict and the 830 figure may have to be revised.
The reasons for high maternal mortality rates are many but it boils down to the low status of women in mainstream Nepali society. Sanchita's case showed how the in-laws delayed taking her to hospital. The disempowerment of girls and women translates into low nutrition levels, early marriage and it results in: delay in deciding to seek medical care, delay in accessing care and delay of care at health centres.
This year, there will be an estimated 900,000 pregnancies in Nepal. Out of these, 129,000 will develop life-threatening complications, according to estimates from the Support to Safe Motherhood Program (SSMP) which the government runs with support from DfID. The program's Indira Basnet told us, "I see maternity mortality more as a human rights and gender discrimination issue than a public health indicator."
Indeed, the interventions needed to reduce Nepal's maternal mortality rate will need to reach beyond just health delivery. Yet, although the number of women dying from pregnancy related complications exceeds the total number of people killed in conflict, safe motherhood has hardly been given priority.
Successive governments have neglected the crisis and been apathetic about better maternal care. Nearly 90 percent of deliveries are still carried out at home under the supervision of friends and untrained traditional birth attendants.
"It is not that Nepal does not have trained health professionals; it does. The trouble is that they tend to be clustered in Kathmandu and other major cities," says Dr Geetha Rana who runs the Women's Right to Life and Health Project at UNICEF. Deliveries without trained birth attendants mean that most women suffer prolonged labour, postpartum haemorrhage and retained placenta. Nearly half the maternal deaths occur due to post delivery bleeding or postpartum haemorrhage.
"Postpartum is the most dangerous period," says Swaraj Pradhan Rajbhandari of USAID's Nepal Family Health Program. Such complications are easily treatable even in district hospitals. The problem is that most rural families constantly delay sending the mother to a hospital. The low standing of the daughter-in-law therefore directly results in her death.
A few years ago, a woman pregnant with her fifth child in Morang suffered internal bleeding after her uterus burst. Her family refused to donate blood. "If she dies, that's her fate," they calmly told the doctor. The husband said: "I'll grow weak if I give her my blood." His wife died within half-an-hour.
"Many mothers don't die due to lack of doctors or medicines, they die because they are not considered important enough," says maternal health expert, Aruna Uprety (See: Column).
According to the Millennium Development Goal, Nepal must reduce its maternal mortality rate from 800 per 100,000 births to 200 in the next 10 years. "What we need most is to raise awareness in the rural areas about safe motherhood practices. It is possible even in this conflict situation," says Ava Darshan Shrestha of the Safe Motherhood Network of groups working in 10 remote districts.
Other countries in the region like Sri Lanka have slashed maternal mortality by doubling the number of skilled birth attendants in the past eight years. The Family Health Division is now following the Sri Lankan model by training skilled birth attendants and setting up birthing centres. The target is to train 752 midwives for the 16 mountain districts, 2,400 in 39 hill districts and 2,400 in the tarai, which has the largest population and the highest fertility rates.
Until now, frontline health care providers have been maternal child health workers. There are 3,152 of them all over the country but they don't fall in the skilled health worker criteria. After 1999, the government tried to upgrade them into Auxillary Nurse Midwives (ANMs) but half of them are ineligible because they do not have adequate formal education. SSMP's Indira Shrestha concludes: "The only hope and the most practical solution is for the government to work with local communities to reduce maternal deaths."
Mothers in numbers
45,000: Number of Nepali women who have died in the past 10 years due to complications at childbirth
12,000: Number of Nepalis who have been killed in the conflict since 1996
6,000: Number of trained midwives needed to reduce maternal mortality
830: Number of Nepali mothers who die for every 100,000 births
92: Number of mothers in every 100,000 births who die in Sri Lanka
2: Number of mothers in every 100,000 births who die in Sweden.


