 Forty years after a successful eradication campaign, malaria is fighting back. Both the mosquitoes and the parasites they carry are getting resistant to antidotes, and have returned to Nepal in an even more virulent form.
Forty years after a successful eradication campaign, malaria is fighting back. Both the mosquitoes and the parasites they carry are getting resistant to antidotes, and have returned to Nepal in an even more virulent form. Malaria is combining forces with other mosquito-borne diseases like the deadly Japanese encephalitis, dengue fever, and kala azar in a compound epidemic across the Nepal tarai. In addition, the effects of global warming could be making it possible for malaria mosquitoes to move up the valleys to higher altitudes.
Although there is a consensus among Nepal's public health specialists that malaria is staging a comeback, there is disagreement about how serious this regression is. Officially, only 50 people die of malaria annually in Nepal and there are 10,000 reported cases. But Govinda Ojha, who is director at the Epidemiology and Disease Control Division of the Ministry of Health, admits: "The actual malaria incidents might be five to ten times more than officially recorded data."

The parasite is transmitted to humans through the bites of infected female anopheles mosquitoes. After spreading rapidly through the bloodstream to the liver, the parasite finally settles in the red blood cells, where it multiplies and bursts out in an explosion of baby parasites. Because of their large numbers, the micro-organisms can damage the nervous system, liver, and kidney.
In young children and adults who have recently been infected, and have not therefore developed natural immunity, this cycle can result in death within hours from cerebral malaria. Others die later of anaemia or liver and kidney failure. Untreated, up to one in five patients infected with the falciparum variety of malaria will die.
Malaria types are named after the strains of the parasites involved, and besides Plasmodium falciparum, in Nepal there is the Plasmodium malariae and Plasmodium vivax. Almost 90 percent of the reported malaria cases are caused by the vivax strain, which causes a relatively benign form of malaria in an otherwise healthy person.
"The possibility of death by vivax is low, and although malaria cases may be under-reported in Nepal, the fatality figures may not be under-reported in the same proportion," explains Prakash Ghimire, a Tribhuvan University specialist in tropical microbiology.
But there are others who are convinced that the threat of malaria in Nepal has been underplayed, and that the disease is about to explode. If that is so, then the country may very well be headed back to 1950s conditions. Jeevan Bahadur Sherchand, an immunologist at the TU Institute of Medicine, and executive director of the Infectious and Tropical Disease Research Centre, says that most malaria deaths are unrecorded since patients are mis-diagnosed as encephalitis or other diseases. Sherchand says: "The government may not want its malaria control programme to be seen as a failure, first to avoid the probable withdrawal of donor funding, and second to protect its international image as a safe tourism destination."
Since the clinical symptoms of malaria are similar to those of other tropical infectious diseases-fevers, chills and headaches-and occur during the same season, many malarial deaths are unreported. At the Shahid Shukra Tropical and Infectious Disease Hospital in Kathmandu, doctors rely less on lab test reports than on "clinical judgement"-when a lab test might not confirm but doctors rely on their experience and judgement to treat patients with newer and stronger malaria drugs. "Approximately 60 to 70 percent of the malaria cases coming to our hospital are treated on the basis of clinical judgement," says the hospital's Shushil Shakya. He explains that obsolete testing equipment and lack of advanced skills among technicians in government hospitals, combined with resistance to popular malaria drugs like chloroquine make the disease untraceable in lab tests, and advise clinical judgment.
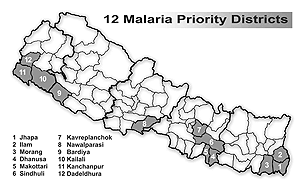
 The government has targeted 12 tarai and inner tarai districts in its anti-malaria campaign. These are priority districts where the rate of transmission is higher, and where there has been a worrying increase in cases of the fatal falciparum malaria.
The government has targeted 12 tarai and inner tarai districts in its anti-malaria campaign. These are priority districts where the rate of transmission is higher, and where there has been a worrying increase in cases of the fatal falciparum malaria. In these districts, infection can be round the year, while in other districts it is seasonal and confined to June-August.
For malaria transmission to take place the habitat of the "transmission area" must support the lifecycle of female anopheles mosquitoes. The temperature must be high enough (16 degrees) to allow the parasite to develop in the body of the infective mosquito, and there must be a pool of infected people in the transmission area that allows the mosquito to pass the disease from an infected person to a non-infected person.
Most of the 12 malaria districts are in the tarai and below 1,000 m in elevation. But warm and wet conditions have helped the disease to spread higher up the valleys. Recent studies by the UN's World Health Organisation show that worldwide, malaria has become an annual epidemic and is spreading to colder climates and higher elevations. Kavre district is in the priority district list because of its proximity to Kathmandu and its higher transmission rate of vivax malaria. The transmission rate in Kavre has increased by almost 40 percent in recent years.
Public health experts are divided about why highland malaria has gained a foothold in Nepal. The explanation ranges from global climate change, to increased movement of people along highways.
Mosquitoes have also developed a resistance to Nepal's favourite insecticide, DDT, which was originally sprayed all across the plains in the 1960s. Sub-standard DDT and lower concentration in sprays in subsequent campaigns allowed mosquitoes to slowly overcome the poison.
It took three decades for the world and Nepal to realise that malaria can be controlled but not eradicated. Between 1955 and 1969 the WHO led a global campaign to try and eradicate malaria from the planet using insecticides and the anti-malarial drug chloroquine. Although some parts of the world were freed from the disease, the WHO has finally admitted defeat. Today, more people die of malaria worldwide than ever before. Ojha at the government's epidemiology division admits: "Completely eradicating malaria is impossible."
 It wasn't just the mosquito that developed a resistance to the insecticide, the plasmodium parasites also became immune to chloroquine. In 1998 the WHO teamed up with the World Bank, UNICEF, and UNDP to launch a Roll Back Malaria (RBM) campaign. The idea was to strengthen health services available to affected populations, and stimulate research and development of new methods to control the disease. The RBM campaign aims to cut the number of deaths from malaria by half by 2010 and by 75 percent by 2015.
It wasn't just the mosquito that developed a resistance to the insecticide, the plasmodium parasites also became immune to chloroquine. In 1998 the WHO teamed up with the World Bank, UNICEF, and UNDP to launch a Roll Back Malaria (RBM) campaign. The idea was to strengthen health services available to affected populations, and stimulate research and development of new methods to control the disease. The RBM campaign aims to cut the number of deaths from malaria by half by 2010 and by 75 percent by 2015. Nepal, too, has changed its strategy to malaria control from malaria eradication. The malaria eradication programme which was funded with USAID support and achieved almost 95 percent eradication was abandoned in the early 1980s when the big donors pulled out. Presently, Nepal spends Rs 90 million annually to control malaria and other tropical diseases.
In Nepal it is lack of awareness, poverty, and misdiagnosis that kills more people than malaria. Kanchhi Maya Gurung from Jhapa was wrongly diagnosed with typhoid and treated with antibiotics that nearly killed her. When her family realised that, after a month of visiting doctors in Jhapa and taking their drugs, her condition was only becoming worryingly worse, they took her to Kathmandu. She is now being treated for malaria and regaining her strength in a private clinic. Kanchhi Maya is one of the luckier ones; thousands of Nepali malaria patients die every year due to misdiagnosis by untrained doctors. Most rural clinics lack microscopes to be able to diagnose malaria from a blood sample.
Then there is the resistance to anti-malaria drugs. "The easy availability of anti-malarial drugs are killing more people because drug resistance is alarmingly high," says TU Institute of Medicine immunologist Dr Sherchand.
A study conducted in Dhanusha in 1996 found that individuals self-diagnose malaria and take the free chloroquine available at the local health post. Village health workers are also allowed to prescribe the tablets without a blood test. After two incomplete courses of chloroquine, the patient is usually not responding to the drug.
Low risk for tourists
Doctors say that although malaria risk is increasing, tourists can protect themselves with proper and timely use of prophylactics.
The CIWEC Travel Medicine Centre in Kathmandu says that the possibility of tourists contracting malaria in Nepal is extremely low. In the 20 years of its presence in Nepal, the clinic has found only two cases of malaria that may have been contracted in Nepal. But a potential visitor to Nepal might face a bewildering array of drugs and varying medical opinion. Tourists coming to Nepal are recommended up to nine different anti-malarial regimes depending on their point of origin or departure.
According to official data more than 60,000 foreigners visit Nepal's southern lowland tarai each year, approximately 83 percent of them going to the Royal Chitwan National Park. The Infectious and Tropical Disease Research Centre in Nepal recommends that those visitors take chloroquine, which is effective against vivax.
The other precautions are using mosquito repellents, sleeping under nets and avoiding getting bitten.


