 |
Wheeze happens when the chest makes strange noises as we breathe in and out. The reason for asthmatic wheeze is that the airways in bronchial asthma narrows and the inhaled air passes the wall of the airway instead of flowing smoothly down the middle.
Narrowing of the airways is brought about when smooth muscles, which line the airways, constrict (broncho-constriction or broncho-spasm is the medical terminology). Broncho-constriction may be caused due to many reasons including cold, allergy, exercise, mental stress and so forth. Therapies have been designed to decrease or reverse this constriction.
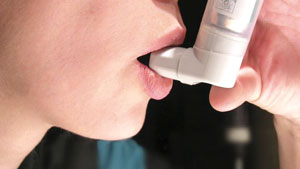
One of the most commonly used medicines in bronchial asthma are beta agonist inhalers which help relax the smooth muscles of the airways and reverse the process of asthma. Asthalin (a common brand name of a beta agonist) inhalers are used commonly and are usually effective. However it is important that the patients learn to use the inhaler properly. Many people do not inhale the medicine but rather swallow the puff of medicine. The medicine goes into the alimentary tract when it was meant to be delivered into the respiratory tract. Or, improper coordination can lead to exhaling air out of the lungs while the puff of medicine is being delivered, which leads to the medicine being wasted into the atmosphere. Beta agonist pills are less expensive but may lead to unwanted side effects.
About 25 years ago, some smart pulmonary scientists determined that relaxing the smooth muscles was just one part in the treatment of bronchial asthma. A revolutionary treatment strategy using inhaled corticosteroids (beclate is a trade name) was put forward because it was clearly shown that persistent asthma had a sizable component of inflammation in addition to the smooth muscle broncho-constriction. Hence, anti-inflammatory medicines in the form of corticosteroids were deployed with startling improvement in asthma care.
It is now routine to add a steroid inhaler if the beta agonist alone is not effective in the treatment of bronchial asthma. Although cold and exercise may be triggers for an asthma attack, travel to high altitude regions amazingly does not seem to worsen existing asthma. This is probably due to lack of allergens at higher altitudes.


