|
|
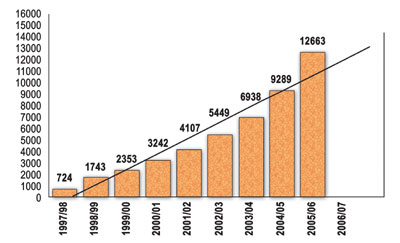
In Nepal, you don't often see graphs as impressive as this one (below), which shows the dramatic line rise in haemodialysis sessions over the last ten years conducted at the National Kidney Centre (NKC).
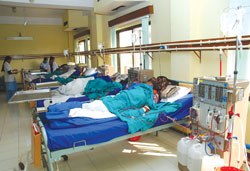
The centre is a textbook example of the progress that can be made in Nepal's healthcare sector despite challenges. From humble beginnings a decade ago-with four hand-me-down dialysis machines and a single rented floor in Putalisadak, the centre now has 30 machines and accommodates nearly 1,400 haemodialysis sessions a month, and has a brand new facility with over eighty staff in Vanasthali.
The centre uses its new facility, originally intended as a hotel, efficiently. As an NGO, it runs primarily on patient fees, with technical support from a group of German organisations and individuals. Overheads are high-in addition to rent, electricity bills run to over Rs 110,000 a month, and the centre uses as much as 30,000 litres of water a day-but the cost of dialysis sessions has reduced from Rs 3,500 per three to four-hour session in 1997 to Rs 2,000 today. The centre also runs an outpatient department for people with kidney problems and follow-ups with transplant patients, and provides heavily subsidised blood and urine tests and ultrasounds. In contrast, the government-run Bir Hospital has just five working dialysis machines. The centre has also donated two dialysis machines to Nepalganj Medical College and three to Dharan's BP Koirala Health Science Institute to run on a non-profit basis.
 Dr Ram Krishna Dulal, the centre's administrative director and public health specialist, says that isn't enough. "I've never seen this kind of growth," he explains. "More are being reported because of increased doctor and patient awareness, but there's also a genuine rise in the number of cases." Dulal suggests that this is largely due to increasingly unhealthy urban lifestyles that contribute to diabetes and hypertension, two major causes of chronic kidney failure. Some 2.6 million Nepalis are estimated to suffer from kidney disease, and there are over 10,000 kidney failures each year.
Dr Ram Krishna Dulal, the centre's administrative director and public health specialist, says that isn't enough. "I've never seen this kind of growth," he explains. "More are being reported because of increased doctor and patient awareness, but there's also a genuine rise in the number of cases." Dulal suggests that this is largely due to increasingly unhealthy urban lifestyles that contribute to diabetes and hypertension, two major causes of chronic kidney failure. Some 2.6 million Nepalis are estimated to suffer from kidney disease, and there are over 10,000 kidney failures each year.
Rather than expanding further, the centre plans to instead spread prevention messages and support centres outside Kathmandu. As the centre's chief nephrologist Dr Rishi Kumar Kafle points out, even the best dialysis facilities are essentially a stopgap. Kidney failure is untreatable, and patients usually need dialysis twice a week to filter blood and remove extra fluid and toxins. This means that even though there are months where NKC conducts over 1,300 dialysis sessions, they're still seeing less than 200 patients. It also means these patients are paying over Rs 210,000 a year for dialysis, just to survive. Lab tests, hormone injections, and medicine for secondary illnesses can double that cost.
"Transplants are the best option," says Kafle, "most people can't support lifetime dialysis, and transplants allow them to become fully productive members of society." The centre, on average, refers two patients for transplants in India every week. Though the procedure is expensive-between Rs 700,000 to Rs 800,000 plus expensive post-op immunosuppresants-the greatly improved quality of life and ability to live without dialysis makes in worthwhile.
The next logical step, say Kafle and Dulal, is to start doing transplants in Nepal. "I'm confident we are competent to do transplants," Kafle says. None of the attempts so far have been successful, but he argues that the major obstacles are more bureaucratic and legal than technical. The Nepali 'Transplant Act' puts doctors at risk of hefty fines and jail time if a patient dies.
Until legislation changes, for patients like 28-year-old former policeman Ramesh Poudel, survival is the focus. A transplant seems unlikely and he's been on dialysis for six years now. He lives alone in Samakhusi and makes the stressful trip to the National Kidney Centre twice a week. "Well, I'm still alive," he says, lying still as tubes of blood run between him and the dialysis machine.